A blog post by Bruce Hamilton; Subscribe at www.oldleandude.com
Last month I joined Eric Buhrens, CEO at Lean Enterprise Institute (LEI) to host a leadership team from the Tel Aviv’s Sourasky Medical Center. They were on a study mission to many of Boston’s fine hospitals and were winding up their week in Boston with a visit to LEI. Early in the discussion one of our guests asked, “In a few words, please tell me what Lean is.” Eric fielded this question concisely, explaining “Lean means creating more value for customers with fewer resources.” He then asked me to relate the following story, a bit more long-winded, to amplify the concept:
I had a recent sojourn of more than a few days at one of Boston’s finest hospitals affording me a rare opportunity for extended direct observation of the process. In Lean lingo, I was observing from the point of view of the “object” of improvement — the
part to be worked on. In a factory, the
object of improvement is a piece of material, a part being progressively converted by
agents of improvement into a finished product.
Clinicians bristle at this analogy. People, after all, are not widgets. Of course, I agree. Patients are each of them unique, and the task to make them well is anything but standard. Caregivers must often make split-second decisions based upon years of experience and practice, spanning an enormous range of different potential conditions. They are indeed agents of improvement, operating singly and as a team, with a passionate commitment to making the patient well. From scrub techs to cleaners to docs, surgeons, nurses, and administrators, these caregivers adroitly shift gears from one minute to next, at one point calming a delirious octogenarian who is screaming in the middle of the night for a pepperoni pizza and then a minute later resuscitating a gentleman in cardiac arrest. As one of their recent customers, I extend my gratitude.
But, as I note in the
Toast Kaizen video,
“continuous improvement is not so much about the work as the things that get in the way of the work.”
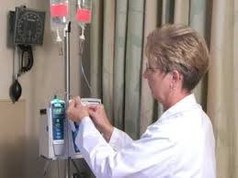
Therefore, please allow me to offer an example from my extended observation. For a period of days, I was tethered to an IV connected by about six feet of plastic tubing to an infusion pump and IV solution bag. The dosage rate required the bag containing the elixir to be replaced approximately twice per day. I say approximately because the flow of medicine was interrupted on average once per hour by a pump fault – an airlock in the line. When an airlock was sensed the pump would pause and alarm. A nurse would then come by to adjust the tubing above the infusion pump, clear the fault and continue the infusion. Depending upon the level of activity on the floor, wait time for the nurse ranged from a minute to fifteen minutes. Oddly, if the fault was not attended to in the first five minutes the alarm grew much louder. This I am told is a countermeasure to “alarm fatigue”, a condition which occurs when there are too many alarms to handle at one time. My sense is that the increased loudness did little more to alert the nurses; it was just an addition to the ongoing cacophony of alarms sounding throughout the floor. In my own case, however, the increased loudness caused me to hit my call button. This sent a signal to the nurse’s station that, after hearing from me that my infusion pump was alarming, would summon the beeper my nurse was carrying. Depending upon the level of the many non-standard things that could be happening on the hospital floor, this might elicit an immediate response – or maybe not.
When the pump alarmed, I understood that my need was not the most critical, but felt compelled to ask my nurse – actually multiple nurses over a period of days – what they thought might be done to reduce the incidence of airlocks in the line; for example, did they think the problem was caused by equipment malfunction or set-up or the viscosity of the solution, or perhaps a software issue? Had they investigated the problem? I was struck by their responses.
First, every nurse assumed that my questions regarding the pump were motivated by my own wellbeing. “No,” I exclaimed, “I’m not asking for myself, I’m inquiring on
your behalf. Your time is so valuable, I hate to see it consumed by these kinds of headaches.” Still, the response was a long-suffering “we do whatever it takes to care for our patients.” In the minds of caregivers, clearing pump faults was just an inevitable annoyance – part of the job. The mindset, while admirably focused on the patient, was also resigned to the status quo of common annoyances. “At what point does an annoyance become a problem?” I asked one nurse. She responded simply “its hard to make changes.” Then, pausing for a second, she reflected, “One of our technicians showed me a trick a while back that he said would reduce airlocks in the line. Let’s give it a try.” With that, she repositioned the tubing above the infusion pump. Subsequently, the pump did not alarm for hours – not until a refill solution bag was needed! The breakthrough here was not so much in the deployment of a potentially better method, but the realization by one caregiver that what she had considered an annoyance was actually a big problem.
Of course, this just a single point of observation, an anecdote. I didn’t see the nurse again to thank her or ask her what trick she had applied. I wondered who else on the floor knew about this trick and how many pointless interruptions to their incredibly valuable work could be reduced if the trick became
a standard.
I concluded my story to the management team: “Your caregivers are your most valuable resource. Management’s job is to create an environment in which the ‘things that get in the way of the work’ are exposed and corrected, enabling caregivers to fulfill their missions with more time and greater focus on making the patient well.”
What do you think? I’d love to hear from you.
O.L.D.